Four of the days during my clinical trial are deemed “insulin sensitivity” days.
On those days, I have to have my meals planned out, and eat them at the same time. Let me clarify what that means: I have to eat the same thing, at the same time, each of those days. Nothing extra, unless I need to treat a low, which I can only do with glucose tabs.
In addition to that, I have to stick to a strict schedule of BG checks during the day. I have to test at least seven times: Before breakfast, lunch, and dinner. Exactly two hours after breakfast, lunch, and dinner. And at bedtime. Since my days also included a snack between lunch and dinner, I checked then too. I also had a snack after dinner, but it was right around the time I needed to perform the post-prandial (after meal) check, so I killed two birds with one stone there.
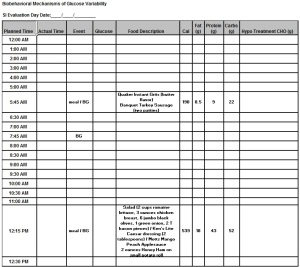
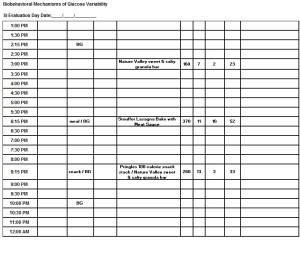
Confused yet? Don’t be. We captured it all on a spreadsheet:
This spreadsheet lists all of my glucose testing and meals for these days. If I needed to treat a low, I added that on. I completed and e-mailed a spreadsheet for each of these days to the research team in Virginia.
Now, the idea with the meal plan was not to eat especially healthy or especially unhealthy. In fact, I was told I could eat whatever I wanted. But once I decided on a plan, it was locked in and I couldn’t change it mid-study. The idea is to measure glucose variability on these days. And by sticking to a regimented schedule of glucose checks and identical carb intake at regular times, the research team would be guaranteed that they’d be testing apples to apples, if you know what I mean.
Regarding the meals: This is pretty much what I’m eating for breakfast and lunch most days anyway. And depending where my BG is, I might or might not have a snack in the afternoon. The hard part for me is that at the end of my workday, I’ve got a 15 minute, half mile walk up the street to the subway, which almost always drops me about 30 mg/dL (Hello Big Blue Test). So I try to be at about 120 mg/dL or so before I leave work (there’s another BG check). On all of these days, even with a snack, I seemed to be low by the time dinner rolled around. Sometimes sooner.
Dinner was definitely different on these days for me. Generally speaking, I do not do boxed dinners. I don’t even eat a lot of frozen processed food of any kind. Not because I’m a health nut. I just find doing my own thing with fresh ingredients is tastier. I know… I really like to live on the edge, right?
These days always reminded me of the early days of my life with diabetes. Inject the same amount of insulin at the same time every day… no exceptions. The diabetic exchange diet… no exceptions. Don’t eat anything more than you’re supposed to. If you do all of these things and you’re not staying in range, it’s your fault. It’s no wonder so many of us got our relationships with food messed up.
The difference here was that I knew these days would end, and I’d go back to a normal way of dealing with my diet. That made going through these days pretty easy, despite the occasional low.
It’s too bad (read: unfair) that some People With Diabetes are still made to feel this way about their eating habits. Diets that give us more flexibility in what we consume, and when, will allow us to figure out what works for us quicker and will allow us to eventually settle to a plan that works for each person individually. We’ll still have our not-so-perfect moments. But the truth is: We had plenty of those with the exchange diet too.
Again, not all studies are like this. It’s just a feature of this particular clinical trial, and I wanted to pull back the curtain a little to show you what it’s like. I think I’ve got one more update to give, probably next week.