Remember that thing I wrote last week about testing the Dexcom G5? It doesn’t look like that’s going to happen. At least not now. There’s a delay in delivery of the device, and it may not be until next year when it can be tested.
I’m finding out that this isn’t uncommon in clinical trials. And my feeling is: Dexcom did a great job developing the G4 and making sure it was ready before it was rolled out. I’m going to trust that there’s a good reason for the delay.
Nevertheless, my study continues. The goal is really designed to test glucose variability anyway, and that can be done with or without a new CGM.
Last week, I made the drive down to Charlottesville for an outpatient visit to the clinical research unit (CRU) at the University of Virginia Medical Center. The team was kind enough to put me up in their research house (where they do outpatient testing of the Artificial Pancreas) so I wouldn’t have to pay for a hotel room.
The next morning, I was at the CRU at 6:30 a.m. I had to be fasting for this test, by the way. Throughout the day, there was a lot of testing going on, but I spent nearly all of my time in a hospital bed, with IVs inserted in both arms.
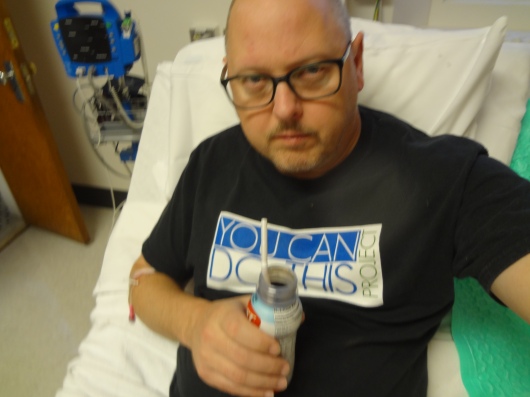
It was a last-minute decision to wear my YouCanDoThis Project T-shirt. I didn’t think much about it when I put it on, but as the day wore on, I think it helped me stay strong. Read on to find out why.
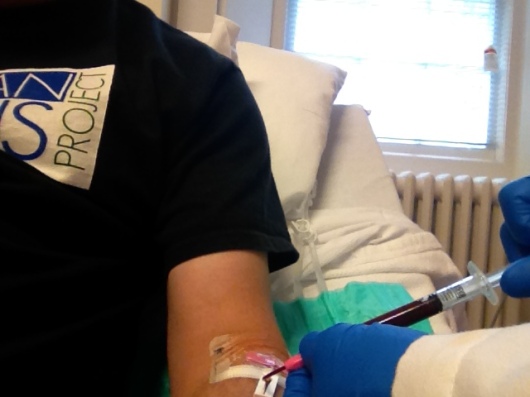
There was a lot of blood drawn from those IVs. Beginning at 7:15, they started taking blood out every 15 minutes. The procedure was the same each time: Use a syringe to draw out a little blood, and discard it. Then draw anywhere from 2 CCs to 5 CCs of blood to give to a technician, who gets two BG readings from the sample. Finally, a third syringe is used to inject saline into the IV, so blood doesn’t dry up in the tubing. That’s why the first syringe was always discarded… probably saline in it, which would change the BG reading.
Dr. Sue Brown was in the room almost all the time too, monitoring my BGs and making sure things were on schedule, and we were able to share cycling stories throughout the morning.
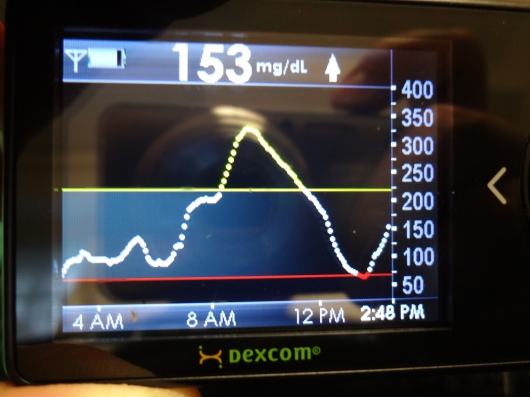
At 8:00 a.m., I was given a carb boost drink (chocolate!), designed to raise my glucose. It took about two hours, but I eventually got up to 297 mg/dL. Once I leveled off a bit, but while I was still high (around 10:00), I received an injection of regular insulin… right into an IV.
Then we waited about two more hours for my glucose to make it down. All the way down to 59 mg/dL. Beginning at 12:00 noon, the team started taking blood out of the IV every 5 minutes until the end of the test at 3:00.
You know, it’s a strange feeling waiting for your glucose to go up, knowing there’s nothing you can are supposed to do about it. But it’s even stranger waiting for your glucose to go down. Feeling the effects of hypoglycemia coming on. Feeling the fog entering your brain, and the world getting smaller, and talking about how you’re feeling while all of it is happening (that was not part of the testing– I just shared).
After that, they gave me a dextrose drink to help me get up to at least 80 mg/dL. Then another. Once I made it over 80 at about 1:30, they fed me lunch. A cheesy, lemon pasta with shrimp, a great salad, and fresh (no, really fresh) fruit for dessert. As you may have imagined, it was delicious. The blood draws and monitoring continued until 3:00 p.m.
So in all, I think there were 56 blood draws, 56 BG tests during my visit. I’ve written about this here so you could get a window into one day of my experience during a clinical trial. They’re not all like this. My previous study didn’t have any days like this.
Like I’ve said before, my job is to help researchers move the needle toward better outcomes for People With Diabetes. If that involves testing a website, or sitting still for intentionally induced hyerglycemia and hypoglycemia, it’s worth it because of what it could mean for those who need better outcomes. If you’ve been considering volunteering for clinical trials, I hope you’ll decide to do it. If you need help getting started, click the E-mail Stephen link on the top left of this page and I’ll point you in the right direction.


Comments
Bravo and thank you. 🙂 (And the blood draws? I have shivers up and down my spine….)
LikeLike
The team was great, and I didn’t feel a thing. But the sheer quantity of the blood draws is what started to wear on me (mentally) after a while. Plus, when you get that insulin into your IV, and you expect your BG to come down, and you still have to wait two hours for it? Kind of surreal, though that may be overstating it. Thanks for the support!
LikeLike
I’m glad you wore the shirt!
It sounds like a physically exhausting trial that turned mentally exhausting as well.
Thanks for doing it for all of us!
LikeLike
Thank you for this. I am glad you wore the shirt too.
LikeLike
Thanks Marie! I think it definitely helped, though it was a good experience overall.
LikeLike
Wow!!! You are amazing for doing this. Thank you.
LikeLike
Wow, you really are amazing…I’m pretty sure I would have fainted from all the blood drawn-I’m getting faint just looking at your photo!
Thanks for doing this for us!!
LikeLike